Many caregivers reach a point where manual transfer of the patient becomes physically unsafe or emotionally stressful. In many cases, this challenge increases as patient mobility declines over time.
Hence, helping someone move from bed to chair or bathroom can quickly turn into a risk for both patients and caregivers. Additionally, back strain, slips, and inconsistent support are some of the common problems that occur in daily care routines.
Fortunately, patient lifts offer a practical solution to this challenge. For caregivers, this also brings a sense of relief and confidence in daily tasks. In such situations, patient handling requires a safer and more reliable approach that protects dignity while reducing physical effort. As a result, mechanical support systems help close that gap by improving stability and control during transfers.
This article discusses the significance of patient lifts, the way they enhance safety, and the areas where they make the biggest impact at home and clinical environments.
1. Safer Transfers Reduced Caregiver Strain
When mobility is limited, manual lifting poses a high risk of injury for caregivers and discomfort for patients. In such situations, patient lifts reduce physical strain and support controlled movement between beds, chairs, and stretchers. As a result, these devices provide mechanical assistance that replaces unsafe manual lifting methods.
The latest discussion on clinical safety notes that mechanical transfer systems significantly decrease the musculoskeletal burden among caregivers. This transition enhances safety outcomes in the workplace, either in home care or in clinical facilities.
The consistent usage of patient lifts also minimizes unpredictable movement during transfers. Sudden shifts that lead to injury are minimized through elevation and lowering. In the long run, this enhances the confidence of caregivers dealing with patients with complex mobility needs. This also supports safer and more efficient handling practices across different care environments.
2. Mobility Support For Patients
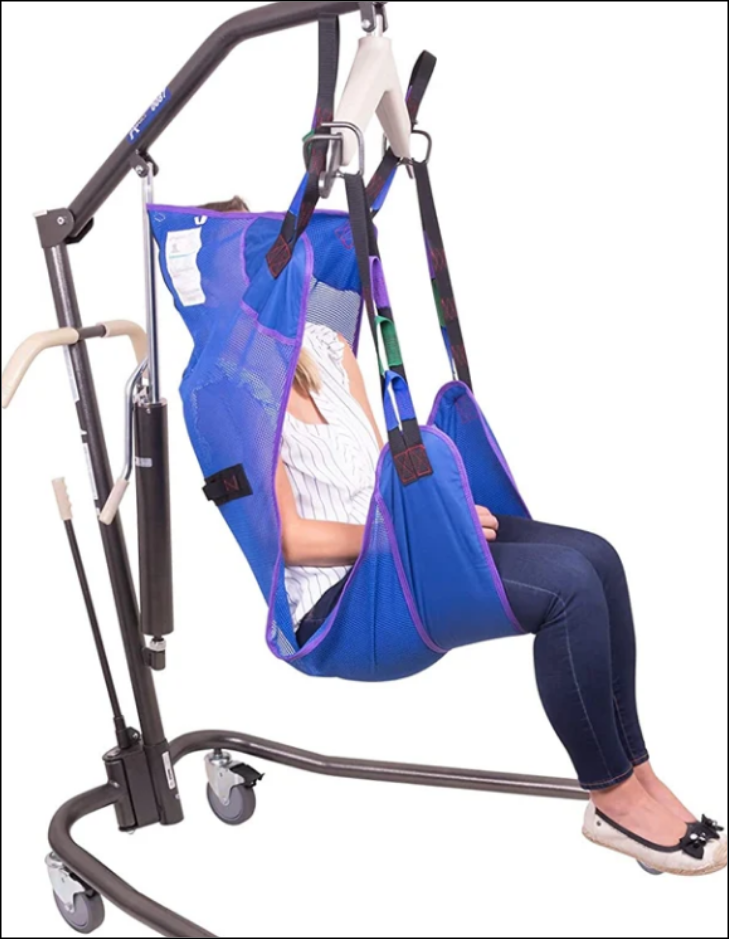
Loss of mobility does not always mean loss of independence. Proper lifting equipment allows patients to participate more actively in daily transitions. This supports dignity and reduces feelings of dependence on manual assistance. Consistent support during movement also helps patients maintain a sense of routine and normalcy in daily care.
The assistive transfer devices can enhance the confidence of mobility and functional engagement in patients with less strength or neural impairments. Better stability in the course of transfers leads to increased movement and increased involvement in everyday activities. It also contributes to progressive recovery of physical ability as a result of harmless rehearsal.
Patients also benefit from reduced fear of falling during repositioning. Secure support systems create predictable movement patterns, which help individuals feel more in control of their body positioning. This psychological benefit is often as important as the physical support itself. Over time, this reassurance can improve willingness to participate in transfers.
3. Fall Prevention in Care Settings
Falls are some of the most common causes of injury, both in home and hospital care. This can be increased in unsafe manual transfers, particularly where the patient lacks balance or strength. Hence, lifting systems to assist the movement include mechanical lifting to even out movement and prevent loss of support.
A review of patient safety interventions reports that structured transfer protocols using assistive devices can reduce fall incidents in long-term care settings. The findings emphasize consistency in transfer technique as a key factor in reducing accidents.
Controlled lifting also helps maintain proper body alignment during movement. This reduces pressure on joints and minimizes disorientation during transfers. Safer positioning leads to fewer incidents of slips and unexpected drops.
4. Improvement in Clinical Workflow

The factor of consideration in healthcare settings is efficiency when staff deal with patients with different degrees of mobility. Traditional handling is hectic and physically straining, which often slows routine care activities. Hence, the use of patient lifts simplifies such procedures by ensuring that the transfer steps are standardized.
Facilities that implement lift systems often report enhanced task flow. Staff can complete transfers with fewer personnel, freeing time for other clinical responsibilities. This improves overall care delivery without compromising safety standards.
Another area of efficiency is reducing fatigue among healthcare workers. Lower physical stress helps maintain consistent performance across shifts. As a result, this can lead to fewer work-related injuries and improved staff retention.
5. Long Term Care Quality
Consistent and safe handling practices are important in a long-term care environment. High levels of transfers need reliable systems that prevent harm to patients and caregivers. Patient lifts offer consistent assistance that minimizes inconsistency in quality of care.
In addition, patient satisfaction and perceived safety during routine care activities are enhanced by the use of structured lifts. Handling consistency will minimize discomfort and establish trust between patients and their caregivers. This reliability is particularly crucial in the case of rehabilitation on a long-term basis.
Over time, better transfer methods contribute to improved overall health outcomes. Reduced injury risk, better mobility participation, and enhanced comfort all combine to raise care standards in both home and institutional environments.
6. Pressure Injury Risk Reduction

The pressure injuries arise due to improper repositioning of the patients or prolonged keeping of the patient in a single position. Automated transfer mechanisms assist in spreading the body weight more equally during the process of movement without placing localized pressure on susceptible locations, including heels, hips, and shoulders. This renders patient lifts a viable instrument in avoiding unnecessary skin injuries both at home and in clinics.
Additionally, structured repositioning supported by mechanical transfer devices can significantly reduce pressure injury rates in immobile patients. The key factor identified across studies is consistency in movement technique and reduced shear force during transfers.
Some of the care environments whose management is mainly through manual handling usually show diverse variability in the quality of transfer. In such cases, patient lifts make movement repetitive, decrease friction throughout repositioning, and aid in the maintenance of safer body positioning. As a result, over time, this consistency supports better skin integrity and reduces complication risks in long-term care populations.
Conclusion
The use of patient lifts is important to enhance safety, mobility, and efficiency in care environments. In addition, they help ease the physical burden on the caregivers and uphold the dignity of patients and the stability of movement. Overall, their value extends beyond convenience into measurable safety and quality improvements.
Furthermore, the implementation of mechanical transfer systems will ease injuries and enhance day-to-day care processes. Whether at home or in the clinic, regular use is effective in developing safer, more predictable, and sustainable care practices. In the long run, adopting these systems supports better outcomes for both caregivers and patients.
Lynn Martelli is an editor at Readability. She received her MFA in Creative Writing from Antioch University and has worked as an editor for over 10 years. Lynn has edited a wide variety of books, including fiction, non-fiction, memoirs, and more. In her free time, Lynn enjoys reading, writing, and spending time with her family and friends.